Introduction
If you’re struggling with pain, mobility issues, or recovering from an injury, there’s no better time to explore physiotherapy in Petaling Jaya. This bustling suburb of Kuala Lumpur is not only known for its lively neighbourhoods and convenient amenities but also for its growing reputation in health and wellness services. Among these, physiotherapy stands out as a holistic and effective approach to managing pain and improving physical function.
Physiotherapy Petaling Jaya clinics offer more than just temporary relief. With skilled practitioners, personalised care plans, and state-of-the-art equipment, physiotherapy here caters to a wide range of needs—from post-surgical recovery to chronic back pain and sports injuries. Whether you’re a professional athlete, a desk-bound worker, or a retiree looking to maintain mobility, the physiotherapy services in PJ are tailored to suit every lifestyle.
As the demand for non-invasive, drug-free treatments grows, physiotherapy is increasingly recognised as a first-line treatment for musculoskeletal issues. Here are five compelling reasons why you should consider trying physiotherapy in Petaling Jaya today.
1. Expert Care Close to Home
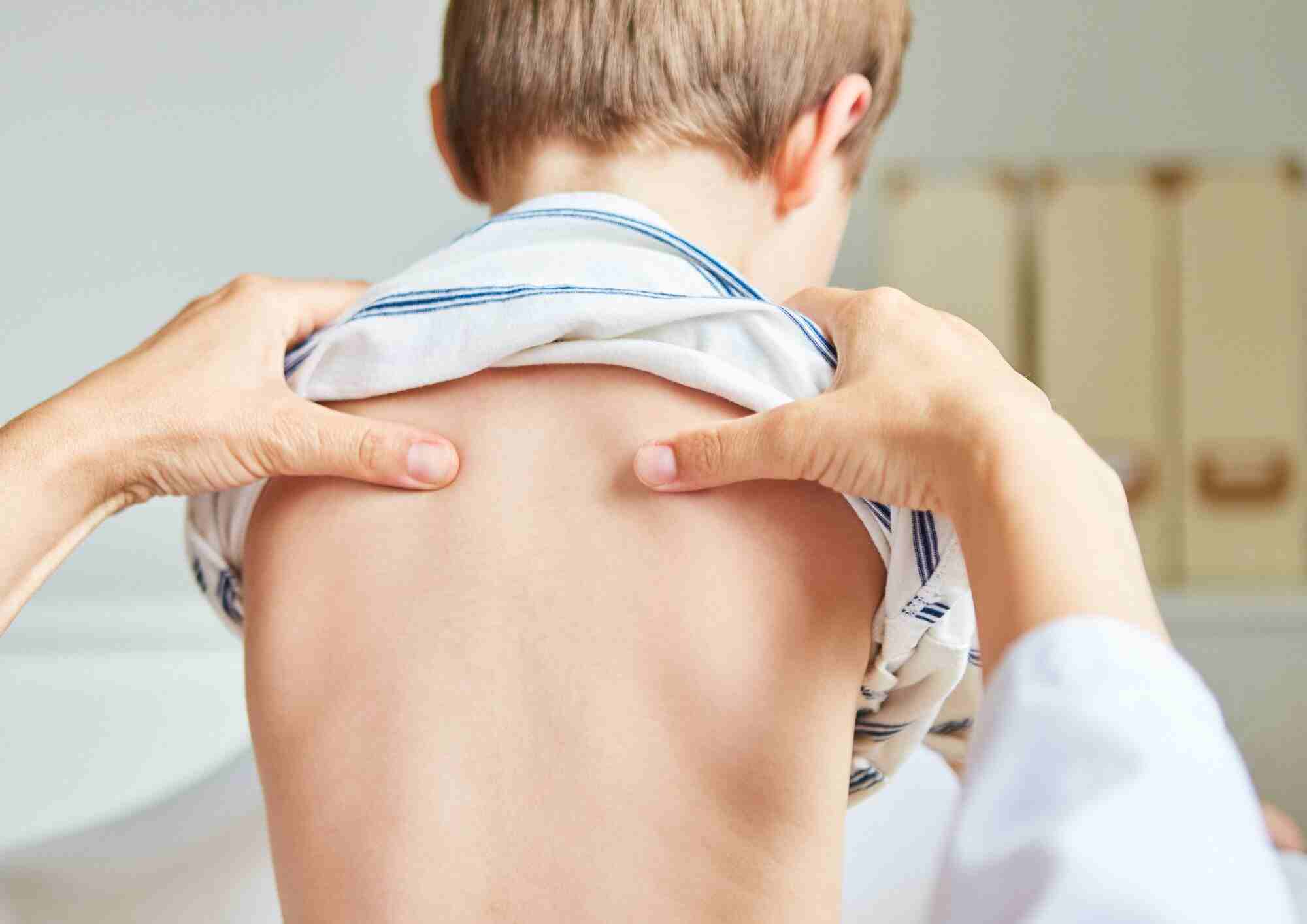
One of the greatest advantages of choosing physiotherapy in Petaling Jaya is the accessibility of high-quality care. The area is home to several reputable physiotherapy centres staffed by experienced and certified physiotherapists. These professionals are trained to assess, diagnose, and treat a variety of physical conditions, from simple sprains to complex neurological disorders.
Specialised Services for Every Need
Many clinics in PJ also specialise in different treatment areas such as sports rehabilitation, orthopaedic physiotherapy, and women’s health. This means you’re more likely to find a therapist who truly understands your condition and can provide targeted treatment to help you recover faster.
Moreover, being located in a central urban area like Petaling Jaya means less time spent commuting and more time focused on healing. You can easily schedule sessions around your work or personal commitments, making it easier to stay consistent with your treatment plan.
2. Personalised Treatment Plans
No two bodies are the same, and the best physiotherapists in Petaling Jaya know that. One of the core principles of physiotherapy is providing personalised treatment that’s tailored to your unique condition, goals, and lifestyle. When you walk into a physiotherapy Petaling Jaya clinic, you won’t get a one-size-fits-all routine. Instead, your therapist will take the time to understand your medical history, lifestyle, and physical limitations.
Targeted and Effective Care
From there, they’ll develop a treatment plan that may include manual therapy, corrective exercises, postural training, electrotherapy, or even ergonomic advice. This personalised approach ensures that the root cause of your issue is addressed, rather than just masking the symptoms.
Such customisation not only improves the effectiveness of your treatment but also empowers you with the knowledge and tools to manage your condition long after your sessions end. If you’re dealing with back pain, for instance, your plan might include spine and core rehabilitation, especially effective for those exploring physiotherapy for slip disc recovery.
3. Effective Pain Management Without Medication
Chronic pain affects millions, and many resort to painkillers for relief. However, prolonged use of medication can lead to unwanted side effects and dependency issues. Physiotherapy offers a safer, long-term solution for managing pain without relying on drugs.
Holistic, Evidence-Based Approaches
In Petaling Jaya, physiotherapists use a variety of evidence-based techniques to reduce pain and inflammation. These can include soft tissue mobilisation, dry needling, therapeutic ultrasound, and exercise therapy. The goal is not just to alleviate pain temporarily but to improve the underlying strength, flexibility, and joint function that may be contributing to the discomfort.
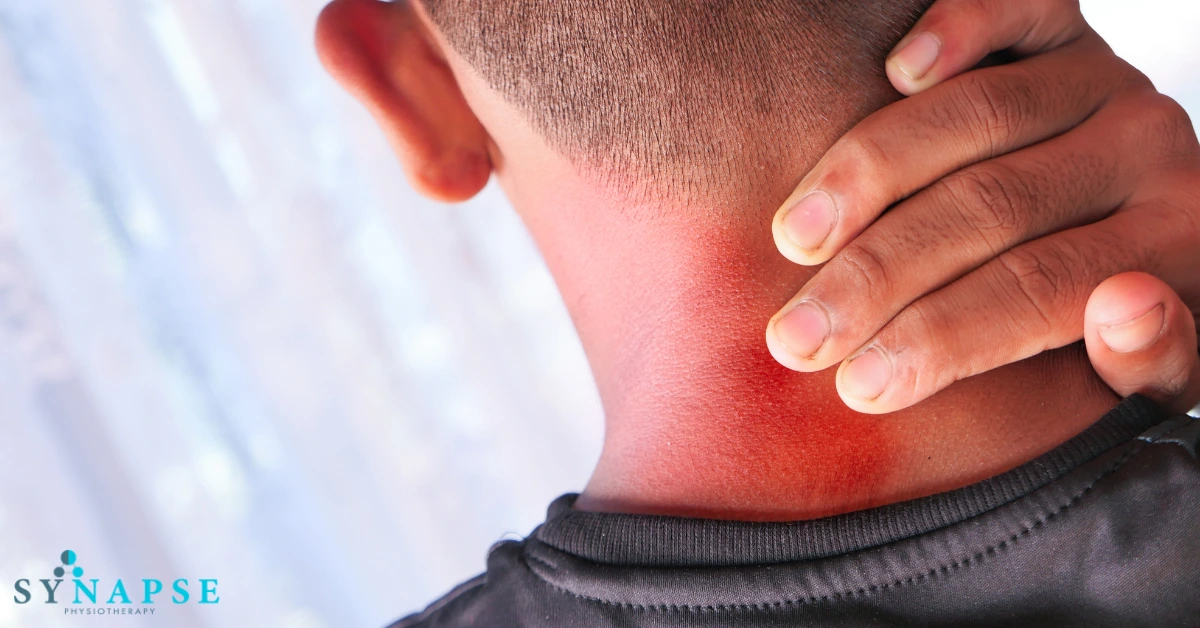
Whether you’re dealing with neck pain from working long hours at a desk or recovering from surgery, physiotherapy can help restore your mobility and reduce pain naturally and effectively. It’s especially valuable for those seeking physiotherapy for slip disc, where long-term improvement is key to avoiding recurrence.
4. Support for Injury Recovery and Prevention
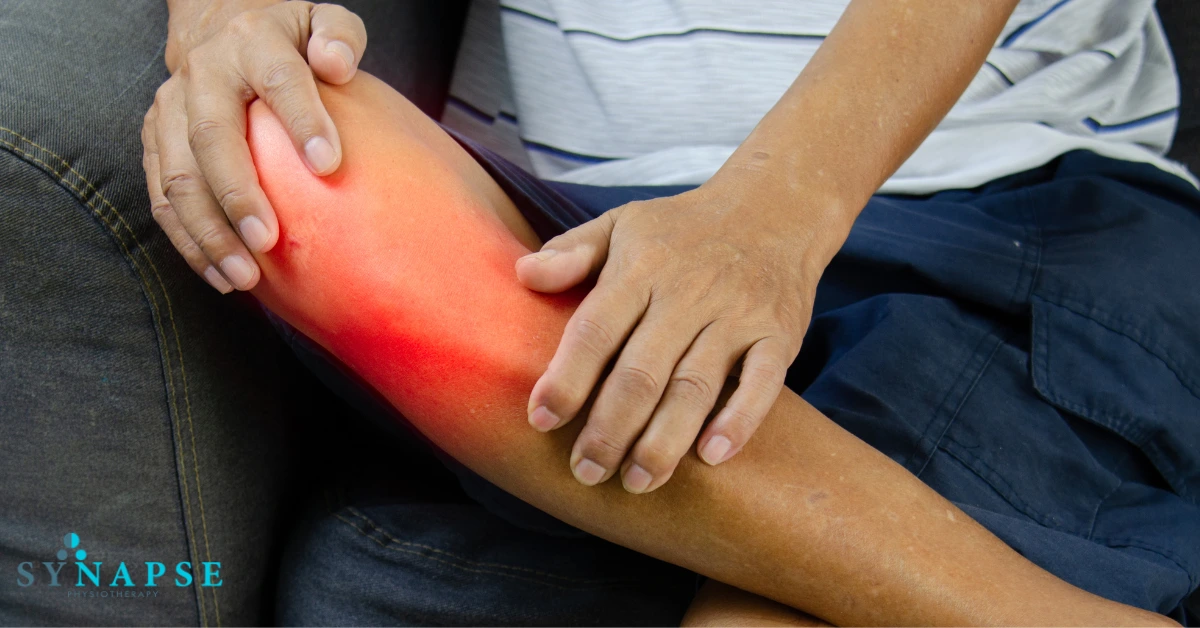
Whether you’re recovering from an ACL tear, a slipped disc, or a shoulder strain, physiotherapy plays a critical role in rehabilitation. Petaling Jaya’s physiotherapy clinics are well-equipped with advanced rehabilitation tools and highly trained staff who can guide you safely through the healing process.
Long-Term Health Benefits
Physiotherapists don’t just help you recover—they also help you prevent future injuries. By identifying movement patterns or muscular imbalances that put you at risk, they can design exercises that strengthen weak areas, improve coordination, and enhance your overall biomechanics.
This is especially beneficial for athletes and active individuals. Many sports teams and fitness enthusiasts in PJ regularly see physiotherapists for maintenance programs that optimise performance and reduce the risk of injury. Furthermore, incorporating strength and conditioning into your routine can enhance these benefits over time.
5. Improved Quality of Life
Physiotherapy isn’t just for people in pain—it’s for anyone who wants to move better, feel stronger, and live a more active life. Regular physiotherapy sessions can help older adults maintain balance and flexibility, office workers counteract the effects of a sedentary lifestyle, and individuals with chronic conditions like arthritis manage their symptoms.
A Holistic Wellness Approach
In Petaling Jaya, the emphasis is often on holistic care. Physiotherapists work not only on your physical health but also educate you on lifestyle changes, posture improvements, stress reduction, and wellness strategies that enhance your overall quality of life.
When your body moves well, everything else follows. You sleep better, feel more energetic, and are more capable of doing the things you love—whether that’s hiking, playing with your kids, or simply walking without pain. This is especially true for those using physiotherapy for slip disc recovery—improved mobility translates directly to improved daily comfort.
Frequently Asked Questions (FAQs)
1. What conditions can be treated with physiotherapy in Petaling Jaya?
Physiotherapy in PJ treats a wide range of conditions, including back pain, sports injuries, arthritis, post-surgical recovery, and neurological disorders. It is also highly effective for managing slip disc issues.
2. Is physiotherapy for slip disc effective?
Yes, physiotherapy for slip disc is one of the most effective non-surgical treatments. It focuses on pain relief, improving mobility, and strengthening the spine to prevent recurrence.
3. How many sessions of physiotherapy are usually needed?
The number of sessions varies depending on your condition and goals. Most clinics in Petaling Jaya offer personalised plans to ensure optimal recovery, especially for chronic issues like a slip disc.
4. Are home physiotherapy visits available in Petaling Jaya?
Yes, many clinics offer home physiotherapy visits for patients who prefer or need treatment in the comfort of their home.
5. Can physiotherapy help prevent future injuries?
Absolutely. Physiotherapy not only aids in recovery but also helps in preventing injuries by correcting posture, improving strength, and addressing muscular imbalances.
Conclusion
Choosing physiotherapy in Petaling Jaya isn’t just a step toward healing—it’s an investment in your long-term well-being. With expert practitioners, personalised care, and a holistic approach, physiotherapy can help you manage pain, prevent injury, and live a healthier, more active life.
Whether you’re facing physical limitations or simply want to enhance your movement and strength, there’s no better time than now to take that first step. Physiotherapy Petaling Jaya has something to offer everyone, so why not explore its benefits for yourself today?
To learn more about how physiotherapy can help with conditions like slip disc, visit our conditions page or check out our full list of rehabilitation programmes.
Tags :

Back & Neck Pain
- Spine & Core Rehabilitation
- Strength & Conditioning Programme
- Pain Management
- Biomechanical Assessment
- Sports Physiotherapy
- Group Class

Sports Injuries
- Strength & Conditioning Programme
- Pain Management
- Biomechanical Assessment
- Sports Physiotherapy
- Shockwave Therapy
- Group Class

Work Desk Injuries

Pre-Post-Surgical Conditions
Scoliosis & Postural Abnormalities

Neurological Conditions

Osteoarthritis & Rheumatism
Joint degeneration and inflammation happens as the human body grows older, but that does not mean our way of life degenerates as well. Relief your joint pains with a joint effort together with your physiotherapist, who will provide pain-relief treatments and prescribe exercises for your wellbeing.

Conditions Relating To Elderly
Common conditions in the older age population include hips & knee pain, back & neck pain, osteoarthritis, rheumatism, fear of falling and many more. Aging and degeneration of bodily function is inevitable, but here at Synapse, we will help you live the best of your life.