Synapse Physiotherapy
What is dry needling
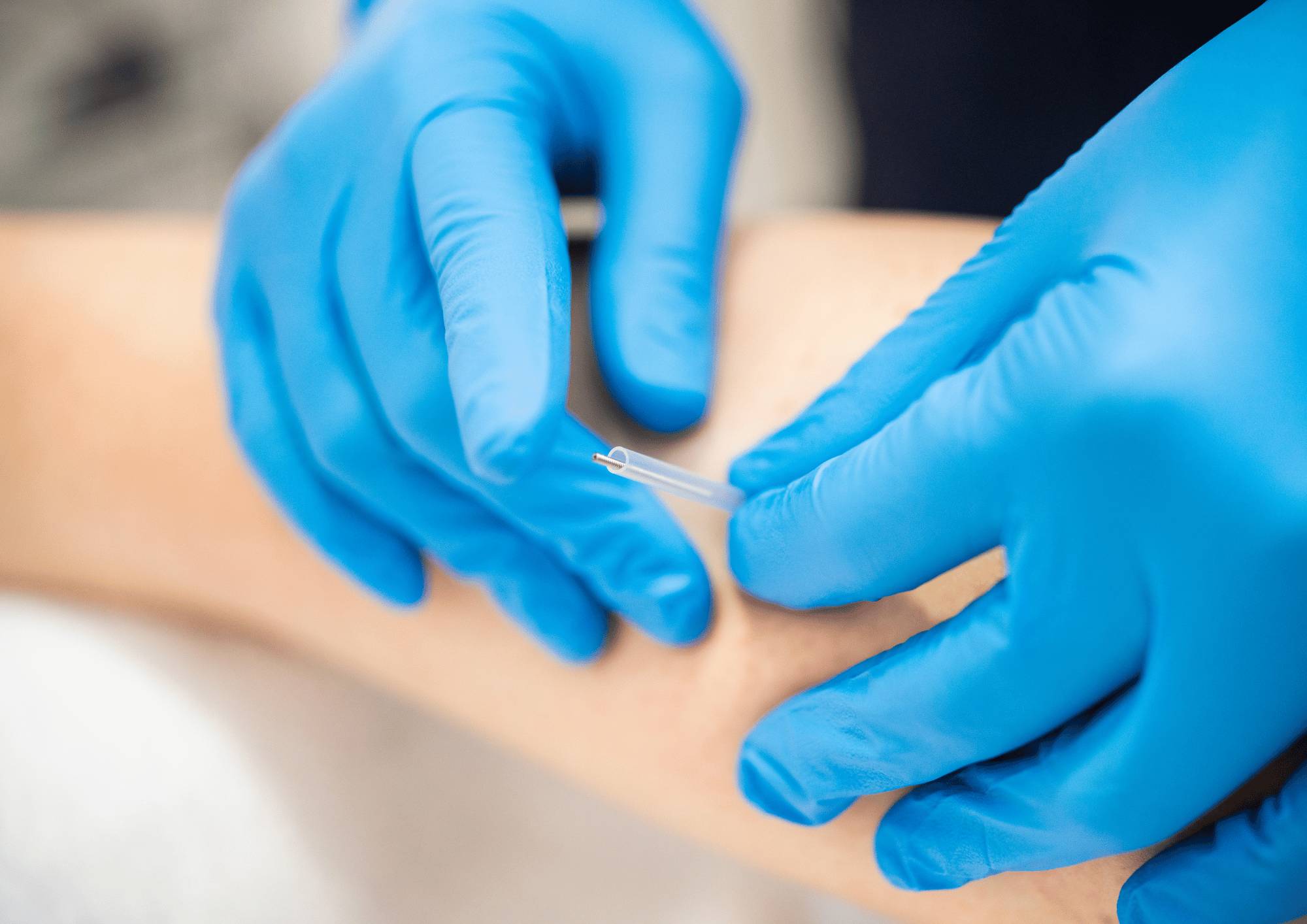
‘Dry needling’ refers to the insertion of thin monofilament needles, as used in the practice of acupuncture, without the use of injectate. Dry needling is typically used to treat muscles, ligaments, tendons, subcutaneous fascia, scar tissue, peripheral nerves, and neurovascular bundles for the management of a variety of neuromusculoskeletal pain syndromes.
National Physical Therapy Association and several State Boards of Physical Therapy\ have recently narrowed their definition of dry needling to insertion of needles into nodules within taut bands of muscle, more commonly referred to as ‘trigger points’ (TrPs) or ‘myofascial trigger points’ (MTrPs)(Dunning et al., 2014).
Differences between dry needling and acupuncture
This question is frequently asked, what is the difference between dry needling and accupuncture. While both therapies utilise solid filament needles, their applications and goals differ significantly. The variations are apparent in the practitioner’s evaluative tools, assessment methods, needle application, and overall objectives. Acupuncture, deeply rooted in Eastern medical traditions and requiring expertise in traditional Chinese medicine (TCM), involves the insertion of needles into specific points along meridians, channels through which the life force or “qi” flows. TCM acupuncture aims to restore the normal flow of this life force.
On the other hand, dry needling (DN) follows a Western medical philosophy, focusing on a practitioner using a thin filiform needle to penetrate the skin and stimulate myofascial trigger points, as well as muscular and connective tissues. DN is primarily employed for managing neuromusculoskeletal pain and addressing movement impairments.
Trigger point
Trigger points are believed to result from an excessive release of acetylcholine from specific motor endplates, categorising them into Active and Latent myofascial trigger points. Active trigger points have the potential to spontaneously initiate local or referred pain, leading to muscle weakness, restricted range of motion (ROM), and autonomic phenomena. In contrast, latent trigger points remain asymptomatic unless stimulated, yet they can influence muscle activation patterns and contribute to limited ROM.
Both active and latent trigger points induce allodynia at the trigger point site and hyperalgesia away from the trigger point when pressure is applied. The formation of trigger points arises from the development of a taut band within the muscle, triggered by an excessive release of acetylcholine from the motor end plate, coupled with the inhibition of acetylcholinesterase and an upregulation of nicotinic acetylcholine receptors.
Initially, taut bands emerge as a normal protective physiological response in the presence of actual or potential muscle damage, often occurring in response to unaccustomed eccentric or concentric loading, sustained postures, and repetitive low-load stress. However, when sustained, these bands contribute to persistent pain.
Pain resulting from trigger points is attributed to hypoxia and reduced blood flow within the trigger point, leading to decreased pH that activates muscle nociceptors in an attempt to restore homeostasis, ultimately causing peripheral sensitisation. Additionally, trigger points play a role in central sensitisation, though the exact mechanism remains unclear. Nonetheless, trigger points perpetuate nociceptive input into the dorsal horn, contributing to central sensitisation.
Mechanism of Dry Needling
Dry needling has demonstrated immediate benefits for individuals with musculoskeletal conditions, showing increased pressure pain threshold, enhanced range of motion, reduced muscle tone, and diminished pain. The efficacy of dry needling is attributed to various mechanisms. Firstly, the procedure induces a ‘local twitch response,’ an involuntary spinal reflex causing localised contractions in the treated muscles, thereby altering the length and tension of muscle fibers and stimulating mechanoreceptors like A Beta fibers. Additionally, dry needling addresses ischemic conditions by promoting vasodilation in small blood vessels, enhancing muscle blood flow and oxygenation. The intervention is also believed to induce neurophysiological effects, prompting local and central nervous system responses that restore hemostasis at trigger point sites and reduce both central and peripheral sensitisation to pain. Moreover, dry needling exhibits remote effects, with evidence suggesting analgesic impacts on proximal Myofascial Trigger Points (MTrP) following needling of distal MTrP.
Contraindication
Absolute contraindications to Trigger Point Dry Needling (TDN) must be approached with a judicious blend of innovation and practicality to ensure the safety and well-being of individuals seeking this therapeutic intervention. Consent denial by the patient stands as a fundamental absolute contraindication, emphasising the necessity of respecting individual autonomy in healthcare decisions. Furthermore, inadequate knowledge or training on the part of the practitioner poses a significant obstacle, highlighting the importance of ensuring a practitioner’s competence through proper education and training. The imperative of uncompromised equipment underscores the need for state-of-the-art tools to guarantee a safe and effective TDN procedure.
Absolute contraindications extend to specific scenarios, such as avoiding TDN during the first trimester of pregnancy, acknowledging the need for caution and consideration of maternal and fetal well-being. Delicate areas like the scalp in infants and sensitive regions including nipples, umbilicus, and external genitalia are rightly safeguarded against TDN due to their vulnerability. Uncontrolled anticoagulant usage poses a potential risk, emphasising the necessity for careful assessment and management of bleeding tendencies.
Equally crucial is the prohibition of TDN over areas with local infection, skin lesions, or active tumors, recognising the potential for complications and the importance of prioritising the patient’s overall health. The occipital region with Arnold-Chiari malformation requires meticulous attention, acknowledging the unique anatomical considerations in such cases. Over a cardiac pacemaker remains an absolute contraindication, highlighting the need for prudence in avoiding potential interference with life-sustaining medical devices (D & David, 2016).
Precautions
Before undergoing Trigger Point Dry Needling (TDN), certain precautions should be carefully considered to ensure the safety and suitability of the procedure for individuals. Individuals with needle phobia or a strong aversion to needles may find TDN psychologically distressing. Those with significant cognitive impairment may face challenges in understanding the procedure, obtaining informed consent, or cooperating during the session. A communication barrier, such as a language difference, may impede effective communication during the procedure. A history of traumatic or spontaneous pneumothorax, hyperalgesia, or allodynia warrants caution, as does the presence of local skin lesions or infections. Patients with compromised immune systems, metal allergies, abnormal bleeding tendencies, or vascular diseases should approach TDN with care, and alternative approaches may need consideration. TDN over surgical implants or in areas of laminectomy requires cautious assessment due to potential risks(D & David, 2016).
Protocol
When performing Trigger Point Dry Needling (TDN), adhere to a streamlined and decisive protocol for optimal efficiency and patient safety. Begin with a thorough examination to identify neuromuscular impairments, ensuring a targeted approach. Confirm the absence of contraindications before proceeding, emphasising the imperative of patient safety.
Secure informed consent from the patient, including a comprehensive disclosure of potential adverse effects associated with TDN. Maintain strict adherence to clean needle technique and universal precautions, incorporating essential measures such as wearing gloves, skin cleaning, and using single-use filiform needles to minimise infection risks.
Identify the trigger point accurately before proceeding with direct needling. Utilise various techniques at the practitioner’s discretion, such as piston motion, to elicit a twitch response. Swiftly and efficiently remove the needle, ensuring proper disposal, and promptly check the patient for any adverse effects.
Following needling, reevaluate the patient’s neuromuscular impairments to determine the immediate effects of the intervention. Conclude the procedure with a decisive introduction of additional therapeutic interventions, such as manual therapy, therapeutic exercises, or modalities, tailored to further reduce impairments and enhance overall function.
This protocol emphasises precision, clarity, and a commitment to achieving definitive outcomes in the TDN process. Strive for efficiency, maintaining a resolute stance throughout each step for the benefit of both practitioner and patient (D & David, 2016).
Frequently Asked Questions (FAQs)
1. What is the difference between dry needling and acupuncture?
Dry needling and acupuncture both involve the insertion of thin needles but differ in their applications and goals. Acupuncture, rooted in Eastern medicine, targets specific points along meridians to restore the flow of life force (“qi”). Dry needling, a Western approach, stimulates myofascial trigger points in muscles, ligaments, and tendons, focusing on neuromusculoskeletal pain management and movement impairments.
2. How does dry needling address trigger points, and what are the effects of trigger points on the body?
Dry needling targets myofascial trigger points, areas of muscle tension. Active trigger points can cause local or referred pain, muscle weakness, restricted range of motion, and autonomic phenomena. Both active and latent trigger points induce allodynia and hyperalgesia. Dry needling’s local twitch response alters muscle fibers, promoting vasodilation, inducing neurophysiological effects, and exhibiting remote impacts, enhancing pain relief and restoring homeostasis.
3. What is the mechanism behind dry needling, and what benefits does it offer for musculoskeletal conditions?
Dry needling’s mechanism includes inducing a local twitch response, promoting vasodilation, and initiating neurophysiological effects. Benefits for musculoskeletal conditions include increased pressure pain threshold, enhanced range of motion, reduced muscle tone, and diminished pain. Dry needling’s effects contribute to both local and central nervous system responses, reducing sensitization to pain and offering immediate relief.
4. Who can benefit from dry needling, and how can I explore these benefits at Synapse Physiotherapy?
Dry needling is suitable for individuals experiencing musculoskeletal pain, myofascial trigger points, or neuromuscular dysfunction. It is often used as a complementary therapy alongside other rehabilitative approaches. To explore the benefits of dry needling with a skilled and professional physiotherapist, you can schedule a session at Synapse Physiotherapy, where tailored dry needling services are offered to address specific needs.
Conclusion
Dry needling may be considered for individuals who are experiencing musculoskeletal pain, myofascial trigger points, or neuromuscular dysfunction. It is often utilised as a complementary therapy in conjunction with other rehabilitative approaches. The decision to use dry needling is typically based on a thorough assessment by a qualified healthcare professional, such as a physiotherapist. You are welcome to explore the benefits of dry needling with a skilled and professional physiotherapist. Synapse Physiotherapy offers tailored dry needling services to address your specific needs whenever you require them.
References
Dunning, J., Butts, R., Mourad, F., Young, I., Flannagan, S., & Perreault, T. (2014). Dry needling: a literature review with implications for clinical practice guidelines. Physical Therapy Reviews, 19(4), 252–265. https://doi.org/10.1179/108331913×13844245102034
D, J., & David, B. (2016). Orthopaedic Physical Therapy Secrets (3). Elsevier Mosby.
Tags :

Back & Neck Pain
Conditions such as stiffness, postural abnormalities and muscle overuse from prolonged desk work at the office or home is more prevalent than most would think. We provide the necessary tools to fix you up and educate you on ergonomics which can unload unnecessary stress.
- Spine & Core Rehabilitation
- Strength & Conditioning Programme
- Pain Management
- Biomechanical Assessment
- Sports Physiotherapy
- Group Class

Sports Injuries
Rolled ankles, jarred knees, impinged shoulders are few conditions in the plethora of sports injuries which can hamper performance and limit our enjoyment of sports. Physiotherapy not only treats the symptoms of these conditions but propels your overall fitness to greater heights.
- Strength & Conditioning Programme
- Pain Management
- Biomechanical Assessment
- Sports Physiotherapy
- Shockwave Therapy
- Group Class

Work Desk Injuries
Conditions such as stiffness, postural abnormalities and muscle overuse from prolonged desk work at the office or home is more prevalent than most would think. We provide the necessary tools to fix you up and educate you on ergonomics which can unload unnecessary stress.

Pre-Post-Surgical Conditions
Surgery involves going through preparation both before and after. Physiotherapists play a vital role in getting your body ready for surgeries with circulatory, breathing and strengthening exercises. After the procedure, let us be there for your recovery and rehabilitation, taking it one step at a time.
Scoliosis & Postural Abnormalities
The way we stand, sit, walk and sleep has influence over our posture and the overall balance of muscles controlling its alignment. A comprehensive screening can be done by our physiotherapists to detect abnormalities, which we will aid in correcting.

Neurological Conditions
Neurological disabilities such as stroke, nerve compression and neuropathies can be barriers for patients to live life to its fullest. We at Synapse are committed to help you overcome these hurdles by ensuring functional mobility and quality of life is at its optimum by providing the right treatment and exercises.

Osteoarthritis & Rheumatism
Joint degeneration and inflammation happens as the human body grows older, but that does not mean our way of life degenerates as well. Relief your joint pains with a joint effort together with your physiotherapist, who will provide pain-relief treatments and prescribe exercises for your wellbeing.

Conditions Relating To Elderly
Common conditions in the older age population include hips & knee pain, back & neck pain, osteoarthritis, rheumatism, fear of falling and many more. Aging and degeneration of bodily function is inevitable, but here at Synapse, we will help you live the best of your life.

Home Physiotherapy
We understand that some conditions or injuries can make it difficult to receive rehabilitation at our clinic be it mobility or transportation issues. Our objective is to provide you with the same high-quality physiotherapy services at home that you would receive in-clinic.
